2016 CAPP Annual Report
OUR VISION
Integrated or organized systems of care will drive movement toward providing superior health care for patients, combining high quality and service with affordability.
OUR MISSION
CAPP promotes the superior performance of our physician-led medical groups and health systems in providing patient-centered medical care that maximizes the quality and duration of life and enhances the health of our patients and entire community.
OUR GUIDING PRINCIPLES
- Integrated (or coordinated) care
- Outcomes-based payment
- Health information technology
- Physician leadership
- Quality measurement
A Message from the Chairman of the Board
The 2016 elections marked the beginning of a time of transition for the nation, including its health care system. While the future is far from certain, we know that change is inevitable. The pressures on physicians and hospitals are likely to increase, regardless of the regulatory and legislative environment. Increasingly, policy experts, elected officials and colleagues in the communities around us will be looking to the highly respected physician-led multi-specialty medical groups that form the Council of Accountable Physician Practices (CAPP) for direction, expertise and solutions. We in CAPP are well-positioned and prepared to provide the kind of leadership the nation needs in these challenging times.
Over the past many decades, the CAPP medical groups have navigated stormy seas while consistently serving as beacons to show the way and models to be emulated. Our members have long been exemplars of how to deliver superior quality medical care in ways that are personal, technologically enabled and effective. All of the CAPP medical directors and Advisory Council members understand that the rising costs and less-than-optimal quality of American health care remain two of our nation’s most critical problems. We share a common belief that CAPP’s five pillars serve as an even more important and powerful foundation for the tumultuous road ahead.
Together, the CAPP groups are focused on finding opportunities to improve the care we provide patients through care coordination, payment reform, access to coverage and physician leadership. We understand that the highest quality outcomes can only be achieved by coordinating all the elements of care and service delivery, and by using advanced information technologies to do so. We also know that the rising cost of prescription drugs in the United States is not sustainable at current levels, and must be addressed before it further harms the health of patients across the nation. As our legislators debate the value of the Affordable Care Act, we urge them to keep their efforts focused on these critical areas of patient care and the importance of the delivery system.
CAPP has made phenomenal progress over the past few years in elevating the voice of the patient and the physician in national conversations and making sure they are heard by policy and political leaders debating the future of American health care.
I appreciate the time you have invested this year in CAPP and the contributions you have made to improving the performance of systems across the country. Doctors, patients and policy experts across the nation are looking to us to demonstrate what is possible through physician leadership. I know that we are ready to answer the call.

Dr. Robert Pearl
Chairman of the Board
The Council of Accountable Physician Practices

A Message from the Executive Director
Last year marked a period of extraordinary growth for CAPP as we continued to fulfill our mission to “state the case” regarding the value of accountable, physician-led health care. In 2016, we attracted attention from major Washington, D.C., policymakers, mainstream and trade media and, most importantly, health care consumers and physicians.
With the support of our CAPP groups and our expert Advisory Council, we hosted two major events in the District of Columbia. Our “Better Together Health” event reached nearly half a million people online. We also continued our research projects to create evidence supporting the superiority of accountable health care. We improved our outreach to attract media print, on-line and social media coverage and solidified our reputation as a highly respected organization, capable of providing insights to peers, colleagues who share our vision and other groups that want to improve.
Our 2017 strategic plan includes a significant investment in engagement and growth as we continue to tell the stories of patients and physicians who thrive inside of CAPP medical groups and as a result of our model of care. We are also increasing our efforts to understand how Americans feel about their health care and explore how we can use this information to encourage progress in delivery system reform.
Thanks for joining us on our journey as we strive to make American healthcare better by working together as one.

Laura Fegraus
Executive Director
The Council of Accountable Physician Practices

2016 Events
Better Together Health 2016
CAPP’s second annual Better Together Health event was held on June 15, 2016, at The Center for Total Health in Washington, D.C. The goals of this annual event are to:
- Raise awareness of the problems with health care delivery system fragmentation and the lack of clinical integration and accountability to highlight the need for sustained efforts around delivery system reform
- Secure interest from health care trade, mainstream consumer and business media to better understand this aspect of health care reform
- Create a public picture of what an ideal system could look like by featuring patient stories from CAPP groups, which specifically showcase the power of coordinated care across a variety of medical group settings and patient conditions
- Raise awareness and enhance the thought-leader reputations of CAPP, its leaders and its partners
This year’s event, titled “Better Together Health 2016: Patient Expectations and the Accountability Gap,” focused on access and coordination of care for patients with chronic disease. CAPP again partnered with Nielsen/Strategic Health Perspectives to survey the American public. This year’s survey sought to determine what aspects of integrated accountable care were actually being experienced by consumers. Results showed a significant gap between what physicians think the system provides and what patients think they get, creating an opportunity to showcase the benefits of the coordinated care model.
Patient Experience Report Card on Coordinated, Accountable Care
Patients with chronic illness do not perceive more coordination of care
Care Team Coordination: Encouraging
About half of patients say that information is still not shared across their providers.

Less than half of physicians say they can share records electronically with providers outside their practice.
24/7 Access to Care: Needs Work
Only about one in three patients thinks they have it.

Only about half of physicians say they provide it.
Treatment Based on Proof: Encouraging
Physicians say they use guidelines… Most patients don’t recall discussions about them
Two-thirds of physicians used evidence-based guidelines to determine treatment
Robust Health Information Technology: Encouraging
More than 1/3 of patients who have online access don’t use it

Physicians are slowly moving to high-tech patient engagement
Prevention in Primary Care: Too Low For Comfort
Fewer than a quarter of patients say their doctor reminds them about prevention and weight loss.
Only about half of primary care doctors say they recommend a weight loss program.
Following the press conference that announced these survey results, the “Better Together Health 2016” event convened. Speakers at this year’s event were:

Robert Pearl
Chair, CAPP

Marc Klau, MD
Southern California Permanente Medical Group

Karen Cabell, DO
The Billings Clinic

Senator Johnny Isakson
(R-GA)

Tim Gronniger
Deputy Chief of Staff, Center for Medicare and Medicaid Services

Leana Wen
Health Commissioner, City of Baltimore

Janet Marchibroda
The Bipartisan Policy Center

Regina Holliday
Patient Advocate

Ceci Connolly (moderator)
Alliance of Community Health Plans
This event also featured patient stories from two CAPP groups, the Billings Clinic and the Southern California Permanente Medical Group.
Event Media Results
Approximately 200 health care policy, media and industry representatives attended the conference in person and via webcast. Survey results from the event attendees continue to be positive:
Our media relations activities around this event generated 34 article placements, which yielded 1,059,695 total estimated impressions.
CAPP is currently planning the 2017 event to be held in Washington, D.C., on May 24, 2017. For more information, please visit the Better Together Health website.
Highlights reels from both the 2016 and 2015 events can also be viewed at Bettertogetherhealth.org.
Physician Leadership in Changing Times
In early 2016, CAPP published a five-part series in Healthcare: Journal of Delivery Science and Innovation on the topic of physician leadership in integrated health systems. This series presented case studies of several CAPP groups based on their experiences with recruiting, retaining and developing physician leadership in their organizations.
CAPP is sponsoring a set of activities to promote the series to foster broader understanding of the way physician leadership can be developed. The first activity was a panel discussion featuring the authors of the series at the 2016 CAPG Washington, D.C., Colloquium.
The panel discussed the series’ findings and implications of this work, putting a spotlight on the need to cultivate physician leadership nationally. The dialogue covered what truly makes a physician leader and highlighted best practices for building a culture that supports physician leadership.
Panelists:
- Dr. Robert Pearl, Chair, Council of Accountable Physician Practices (moderator)
- Dr. Lee Sacks, Advocate Physician Partners
- Dr. Philip Oravetz, Ochsner Health System
- Dr. Nick Wolter, Billings Clinic
- Dr. Marc Klau, Southern California Permanente Medical Group
CAPP 2016 Advisory Council: Health Care in the New Political World
On November 30, 2016, a group of 30 CAPP Advisory Council members and Medical Directors met in Washington, D.C., at the Kaiser Permanente Center for Total Health to discuss implications of the 2016 presidential and congressional elections on future health care policy. Health care futurist Ian Morrison moderated a discussion with political analysts Dean Rosen and Chris Jennings and Politico Executive Editor for Healthcare Joanne Kenen. In the afternoon, the attendees heard a presentation by Rob Mechanic of Brandeis University about his research into CAPP group readiness for payment reform. The meeting attendees also discussed CAPP’s strategic direction and plans for 2017.
2016 Media Activities
Media Relations
Since 2014, CAPP has retained Scott Public Relations as our media relations partner. The firm’s charge is to generate and elevate awareness, interest, and informational requests from trade and mass media about CAPP, CAPP messages, blogs and activities. The intent is to advance CAPP, AMGA and the AMGA Foundation as the leading industry representatives in matters of health care delivery reform and integration, physician leadership and health care payment reform.
Other 2016 Communications and Media Activities
- CAPP once again exhibited at the Association of Health Care Journalists’ annual conference, reaching national and local health care journalists from media outlets around the country.
- The CAPP-produced white paper and primer, “What Every Candidate Should Know About Health Care,” provides health care media with physician and medical group perspectives on what the critical issues are in health care reform to encourage them to dive deeper than shallow analysis of the Affordable Care Act. The primer was released in August 2016 and focuses on payment reform, health care IT use and quality measurement.
- In addition to the Accountable Docs blog and social media activities, CAPP produces tools to help physicians and policymakers understand accountable care. Following CAPP’s 2015 release of a whiteboard video explaining “What Is Accountable Care?”, in 2016, CAPP produced a second video to explain what it means for a physician to work in an accountable coordinated care setting. “A Day in the Life of an Accountable Doctor” was produced to further educate and engage physicians on the ideal concept of “accountable care.” This video will premiere in early 2017.
- Man-on-the-Street Video: CAPP recently conducted a two-part pilot project to capture the voice of the average patient. CAPP interviewed 16 passersby at the Grand Lake Farmers Market in Oakland, CA, and 13 residents of Billings, MT, on video about their thoughts on accountability in healthcare.
Overall CAPP Media Coverage
(Oct. 2014 – Dec. 2016)
Total number of articles/media placements to date:
100
Total number of impressions:
76,042,331
Outreach to
100+
national and trade media to introduce CAPP as a resource
2016 Research Projects
Brandeis Capitation and Salary Study

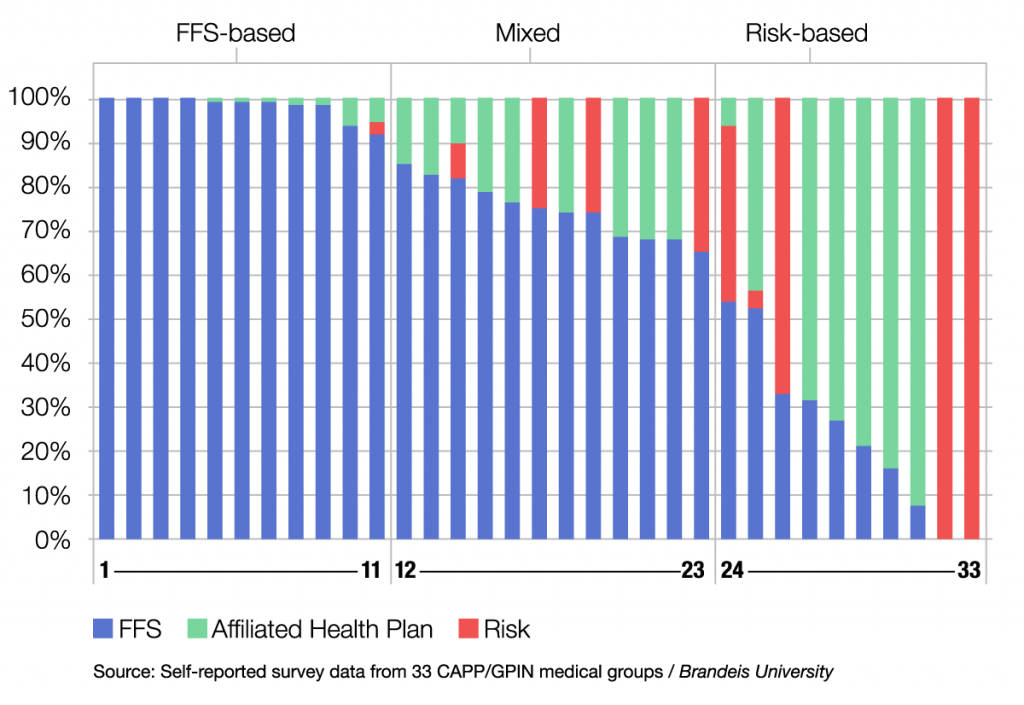
Many policy analysts have advocated for modifying current methods of paying for medical services away from fee-for-service and towards bundled payments for defined episodes of care or global capitation. In collaboration with Brandeis University, CAPP launched a project to estimate the prevalence and magnitude of capitation and other alternative payment contracts among CAPP’s organized physician groups, which would provide a barometer of the “readiness” for payment reform among organized medical groups.
The final results of the first study were published in the September 2012 issue of Health Affairs. In that paper, “Many Large Medical Groups Will Need to Acquire New Skills and Tools to Be Ready for Payment Reform,” authors Robert Mechanic and Darren E. Zinner found fee-for-service to be the dominant payment method among the surveyed groups. In 2014, the researchers updated the survey. These results were presented at the Health Industry Forum in Washington, D.C. on April 2, 2015 and were published in July 2016 in the American Journal of Managed Care. The research implications were published on the Accountable Docs blog here.
CAPP and Brandeis are currently conducting a third round of this survey, which will draw on the same sample as the second. This ongoing project will allow us to track payment reform progress and provide both real-time analysis and consistent historical accounting of the “pay for value” movement.
Revenue by Patient Model and Group Category
Mixed (n=12)
Risk-Based (n=12)
Physicians Foundation IDS Research
To better understand physician-led integrated delivery systems (IDS) and independent practice associations (IPA), The Physicians Foundation sponsored a CAPP research project to identify case examples of successful physician-led IDS/IPAs. The research has been completed. Dr. Lawrence Casalino of Weill Cornell was the lead researcher and has co-authored the resulting paper with Dr. Norman Chenven of Austin Regional Clinic. The paper, “Independent Practice Associations: Advantages and Disadvantages of an Alternative Form of Physician Practice Organization,” was published in Healthcare: Journal of Delivery Science and Innovation in September 2016.
Leadership
CAPP Board of Directors
Chairman:
Robert Pearl, MD The Permanente Medical Group and the MidAtlantic Permanente Medical Group
Vice-Chairman:
Norman Chenven, MD The Austin Regional Clinic
Secretary:
Steven Green, MD Sharp Rees-Stealy Medical Group
Treasurer:
Ira Nash, MD Northwell Health
Liaison:
Donald Fisher, PhD The American Medical Group Association
Al Fisk, MD The Everett Clinic
Robert Nesse, MD The Mayo Health System
Philip Oravetz, MD Ochsner Health System
Robert Pearl, MD The Permanente Medical Group and the MidAtlantic Permanente Medical Group
Norman Chenven, MD The Austin Regional Clinic
Steven Green, MD Sharp Rees-Stealy Medical Group
Ira Nash, MD Northwell Health
Donald Fisher, PhD The American Medical Group Association